In this section
Alongside the available resources, implementation support is critical to ensure that there is systematic and sustainable implementation of the frameworks. Having systematic support will enable all practices in an area to implement the frameworks consistently, reducing the likelihood of exacerbating existing health inequalities.
Access our UCLPartners Proactive Care Framework Implementation Workbook
Essential Pillars of implementation
These frameworks are designed to be adapted to local context and preferences. From our experience of spreading health and care innovations and working in primary care, we recommend the following six essential pillars to ensure successful local adaptation:
- Strategic engagement – system leaders, community partners and patient involvement
- Local clinical engagement to question, understand and adapt the frameworks to local context, supported by UCLP resources
- Supporting workforce transformation
- Identifying key roles to deliver the frameworks
- Conducting a training needs analysis for these roles
- Training for additional roles to deliver the proactive care interventions
- Mobilise levers to drive forward primary care transformation e.g. alignment of local incentive schemes
- Defined data collection including setting key metrics to measure progress and impact
- Governance and project management that drives the work forward and allows agile decision making
Approach for implementing Proactive Care Frameworks
Driven by cardiovascular and respiratory disease and to get the economies of scale by sharing resources across practices. To achieve the population health benefits and reduce health inequalities driven by cardiovascular disease, we recommend implementing the frameworks at a PCN level. There are four key phases of implementation to deliver the Proactive Care Frameworks at an ICS or PCN level.
Within the Implementation section of the website, guidance and key resources are provided for each of the phases of implementation.
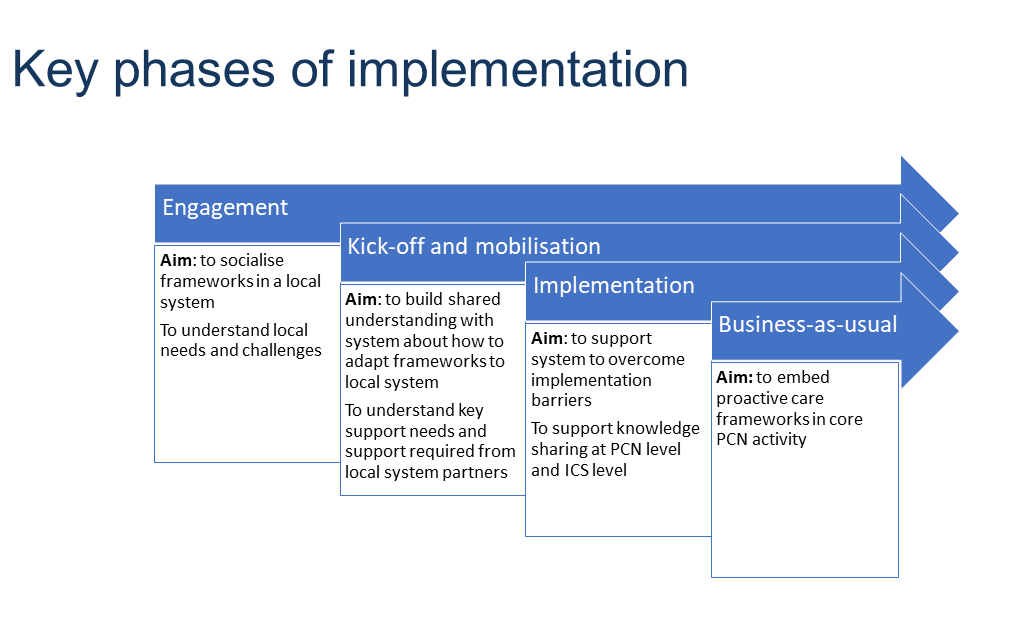
Implementation support for partners in the UCLP Geography
For Primary Care teams within the UCLPartners footprint, we can provide support to improve the quality of proactive care for patients with long-term conditions. We can offer expertise from across our organisation including experienced GPs, clinical pharmacists, project managers, implementation and quality improvement experts. Our team can provide the following types of support, all of which can be tailored to the needs of your context:
- Programme/project management to adapt and embed the frameworks in Primary Care Networks
- Support for local clinical engagement and leadership
- Adaption of the frameworks to reflect local pathways
- Workforce training and education including:
- Communications training and support – encompassing motivational interviewing and health coaching principles to support the primary workforce to deliver the protocols.
- Best practice in virtual consultations – practical training and support to deliver high quality remote consultations.
- Condition-specific training – collaboration with local Training Hubs to provide training on each of the conditions covered by the frameworks.
- Digital and tech resources to support remote care and self care
- Data collection and evaluation support
We are working closely with North Central London Clinical Commissioning Group and North East London Commissioning Alliance as part of a national pilot funded by NHS England and Improvement’s Proactive Care @Home programme. Read out top tips from implementing the frameworks from our partners in NCL.
If you are based within the UCLPartners geography, please contact us at primarycare@uclpartners.com
If you are not based within UCLPartners’ geography, please remember all the resources are freely available from this microsite. For implementation support, please contact your local AHSN.
Implementation workshops
Join us for an interactive, informative online workshop for all health and care colleagues involved in primary care transformation. The UCLPartners clinical and education teams will explain what the Proactive Care Frameworks are and how to make the most of the Implementation workbook to start using the Frameworks effectively to improve patient care today. Find out more and sign-up for the workshops